Observations of mice engineered to carry a mutation that causes a severe form of dwarfism have led to a better understanding of the pathology of the disease and potentially identified a window during which treatment may be most effective. The study, which was funded in part by the NIH’s National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), was published in the Journal of Bone and Mineral Research.
Pseudoachondroplasia (PSACH) is a disorder of the growth plate that results in dwarfism, limb deformities, joint pain, and early onset osteoarthritis. Children with the disorder show no signs of it at birth, but by age 2, symptoms such as slowing of long bone growth and a waddling gait begin to appear. The disorder is caused by mutations in the cartilage oligometric matrix protein (COMP), which is found in the intricate lattice of proteins and other molecules that forms in the spaces between cells (extracellular matrix). COMP is situated near cells known as chondrocytes, which play a key role in bone formation. The protein binds cartilage components together.
Previous studies of PSACH have been limited, relying on PSACH cells grown in the laboratory or samples taken from human biopsies, and have not led to the development of feasible treatment options. Researchers recognized that they need a better method to study the disorder.
“We generated a mouse that carries the human COMP gene that contains the most common mutation in PSACH. Similar to how the disease manifests in humans, these mice appear normal at birth, but later show symptoms of PSACH, giving us a unique opportunity to potentially pinpoint when changes occur and when treatment may be most effective,” said first author Karen Posey, Ph.D., of the University of Texas Medical School at Houston, who collaborated with NIAMS grantee Jacqueline Hecht, Ph.D., on the project.
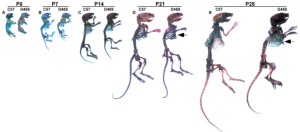
Posey and her colleagues examined the mice at different stages of development to track the disorder’s progression. They found that about two weeks after birth (which equates to about four years in humans), chondrocyte cells begin to die, and the symptoms of the disorder begin to be expressed. They also found inflammation in the growth plate and cartilage of the joints, suggesting the beginning of osteoarthritis.
To determine if there was a potential way to reduce the effects of the disorder at its earliest stages, the researchers administered three different medications to the mice beginning at birth—lithium, phenylbutyric acid and valproate. These medications typically are used to treat mood disorders, but they are also thought to reduce cellular stress. They found that the drugs successfully lessened the damage to chondrocyte cells in the growth plate, but each drug resulted in significant side effects, including skeletal defects and early death. Nevertheless, the results showed promise.
“Although these drugs in particular are not viable treatment options, our findings do provide a foundation for the development of a therapy that would reduce inflammation in the growth plate chondrocytes,” said Posey. “We also identified an optimal treatment window for children—starting around age 2, when most of the cells in the growth plates are still viable and widespread cell death has not yet occurred. Once growth plate chondrocytes have been depleted, treatments likely would have little effect,” Posey concluded.
The research reported in the article was supported in part by NIAMS grant number R01AR057117, awarded to the University of Texas Medical School at Houston and Dr. Hecht.
Posey KL, Coustry F, Veerisetty AC, Liu P, Alcorn JL, Hecht JT. Chondrocyte-Specific Pathology During Skeletal Growth and Therapeutics in a Murine Model of Pseudoachondroplasia. J Bon Miner Res. 2014 May. 29(5): 1258-1268.
